| Table of Contents |  |
|
Original Article
| ||||||
| A study of etiology and prognosis of oculomotor nerve paralysis | ||||||
| Maraiah Pradeep Kumar1, Undrakonda Vivekanand2, Shashikiran Umakanth3, Yashodhara BM4 | ||||||
|
1Associate Professor, Department of Ophthalmology, Shimoga Institute of Medical Sciences, Karnataka, India.
2Associate Professor, Department of Ophthalmology, Alluri Sitarama Raju Academy of Medical Sciences, Eluru, West Godavari District, Andhra Pradesh, India. 3Professor, Department of General Medicine, Department of General Medicine, Melaka Manipal Medical College, Manipal, Karnataka, India. 4Associate Professor, Department of General Medicine, Melaka Manipal Medical College, Melaka, Malaysia. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Kumar MP, Vivekanand U, Umakanth S, Yashodhara BM. A study of etiology and prognosis of oculomotor nerve paralysis. Edorium J Neurol 2014;1:1–8. |
|
Abstract
|
|
Aims:
To study the etiological pattern and prognosis of oculomotor nerve palsy in a medical college hospital in South India.
Methods: This study comprises 40 cases of oculomotor nerve palsy presenting to medical college hospital between March 2004 to September 2005. Details of various modes of presentation, aetiologies, pupillary involvement and recovery were documented and analysed. Conclusion: Isolated oculomotor nerve palsy which is a predominant mode of presentation has a good recovery rate. We recommend that patients with oculomotor nerve palsy be carefully examined clinically in close collaboration with other specialists, especially where sophisticated complementary investigations are impossible. | |
|
Keywords:
Oculomotor nerve palsy, Outcome, Partial, Management
| |
|
Introduction
| ||||||
|
Etiological trends of oculomotor nerve palsy have remained fairly consistent over the decades, although there is a changing disease pattern worldwide and the current focus is on etiologies like diabetes, trauma and orbital inflammatory diseases which are emerging as frequent causes of third cranial nerve paralysis. [1] [2] Thus a collaborative approach with other specialties is essential to enhance the diagnostic accuracy. This study reports the results of clinical, etiological and prognostic aspects of oculomotor nerve palsy using such a collaborative approach. | ||||||
|
Materials and Methods
| ||||||
|
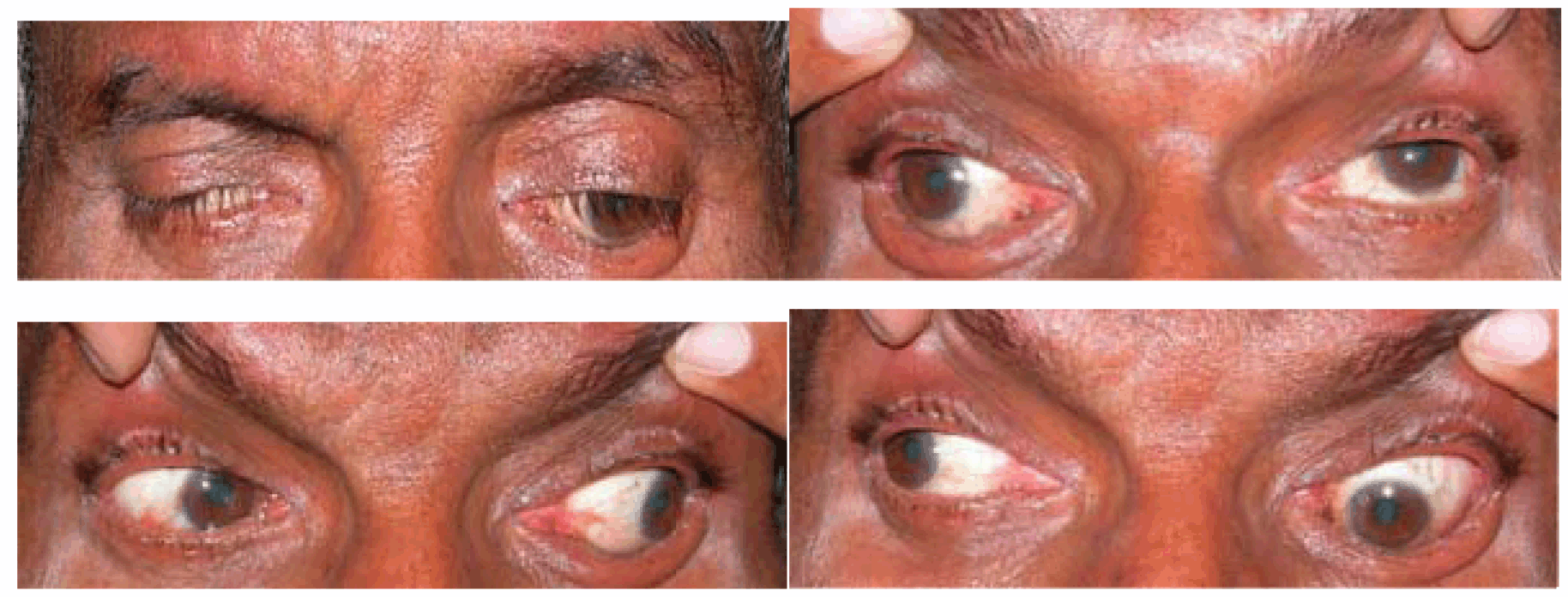
The study population consisted of 40 consecutive cases with acquired oculomotor nerve palsies, who were referred to neuro-ophthalmology outpatient department at Krishna Rajendra Hospital (KRH), Mysore, Karnataka from March 2004 to September 2005. All patients with oculomotor nerve palsy were who diagnosed clinically and documented appropriately with Hess charting and diplopia charting were enrolled for the study. The inclusion criteria were: i) Acquired oculomotor nerve palsy with a recent onset (within two weeks) ii) Oculomotor nerve palsy associated with other neurological signs and symptoms other than the palsy itself. iii) Informed written consent. Cases of congenital oculomotor nerve palsy, myasthenia and other myopathies, isolated fourth nerve and isolated sixth cranial nerve palsies and patients presenting later than six months from the onset of third cranial nerve palsy were excluded from this study. A detailed current and past medical history of the subjects was taken. Documentation included age, gender, detailed history focusing on present and past medical status, best corrected visual acuity as Snellen's fraction values. A comprehensive ocular examination and slit lamp biomicroscopy was performed in all the patients. Particular attention was paid to lid examination, pupillary reflexes, and extraocular movements. Ptosis, if present, was graded. Ptosis was considered present when the eyelid aperture of one eye was >1 mm smaller than the other. Ptosis was further classified into mild (<2 mm), moderate (2–4 mm) and severe (4–8 mm). Pupils were checked for size, shape, and light reflexes. Pupillary involvement was checked by measuring the pupil size and its reactivity to light. Standardized methods were used to measure pupil size. Patients were instructed to look at a target kept six meters away under stable room light conditions. A millimeter ruler was used to measure the pupillary diameter to the nearest 0.5 mm. The normal pupillary diameter was standardized to 3 mm. The patients were engaged in conversation to ensure that they were alert. The degree of anisocoria, if present, was recorded. Physiological anisocoria was ruled out after repeating the measurements in dim light. Hess charting and diplopia charting were done in all cases to confirm oculomotornerve palsy. Degree of ophthalmoplegia was quantified by recording the relative limitation of ocular ductions of the superior, inferior, and medial recti muscles and inferior oblique muscle using a 0 to 4 scale. [3] Grading was done as: 0 represented full duction; 4 complete absence of function; and 1, 2 and 3, 25%, 50% and 75 % impairment of duction, respectively. A single ophthalmoplegia grade was determined by calculating the arithmetic mean of the relative limitation of ocular ductions of the involved four muscles. A detailed systemic and neurological examination was done in each case with special emphasis on cranial nerves examination. Besides routine blood investigations, blood pressure measurement, random blood sugar, erythrocyte sedimentation rate and serum cholesterol, other procedures like mantoux test, CSF analysis, radiological examination of skull, orbital fissures, optic foramina, paranasal sinuses, computed tomography, and car-otid angiography were performed wherever indicated. All patients were reviewed again after two weeks and eight weeks from the baseline visit. Lid position, extra-ocular movements, pupil size, and reaction to light were recorded at every visit. The data collected from the patients were tabulated and the results of the analysis are presented in the tables. | ||||||
|
Results | ||||||
|
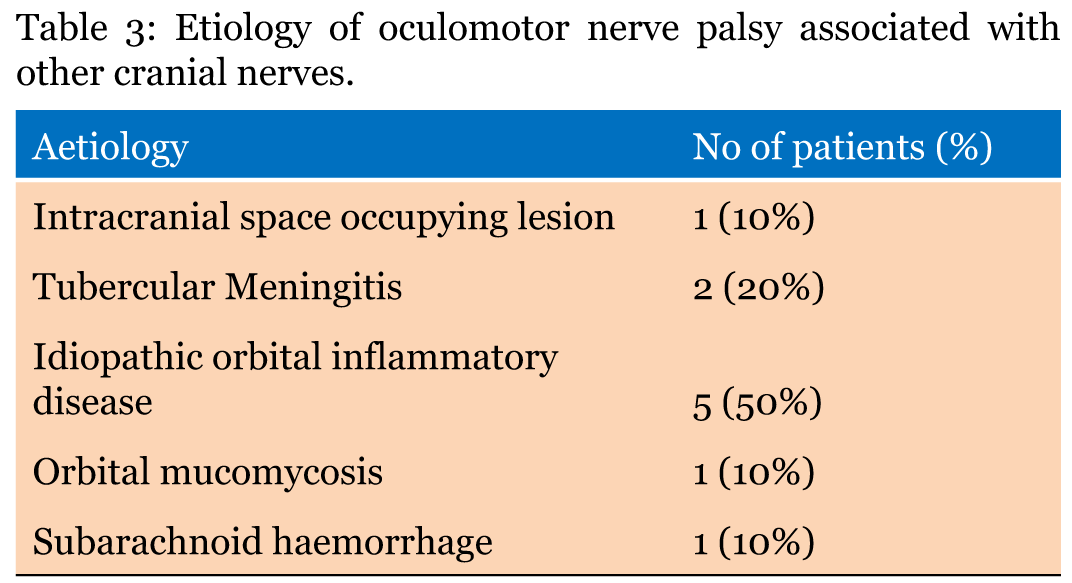
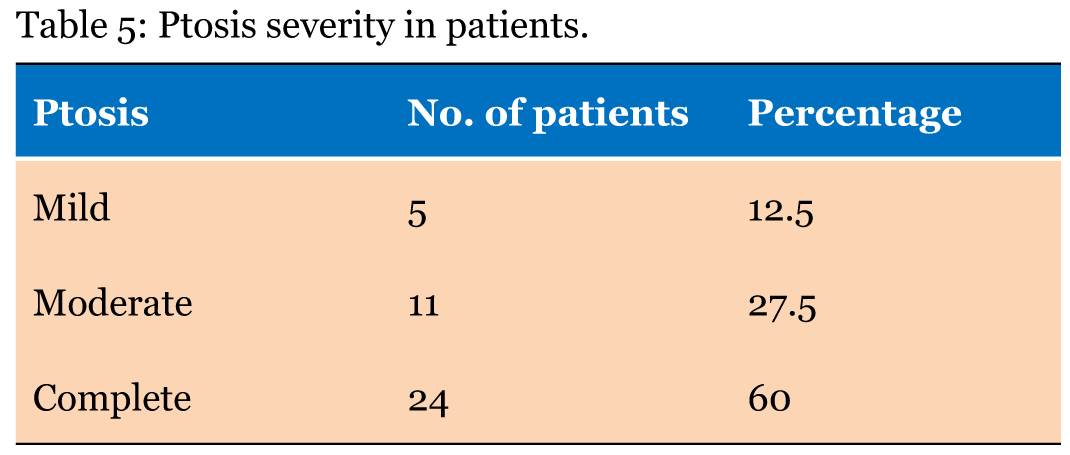
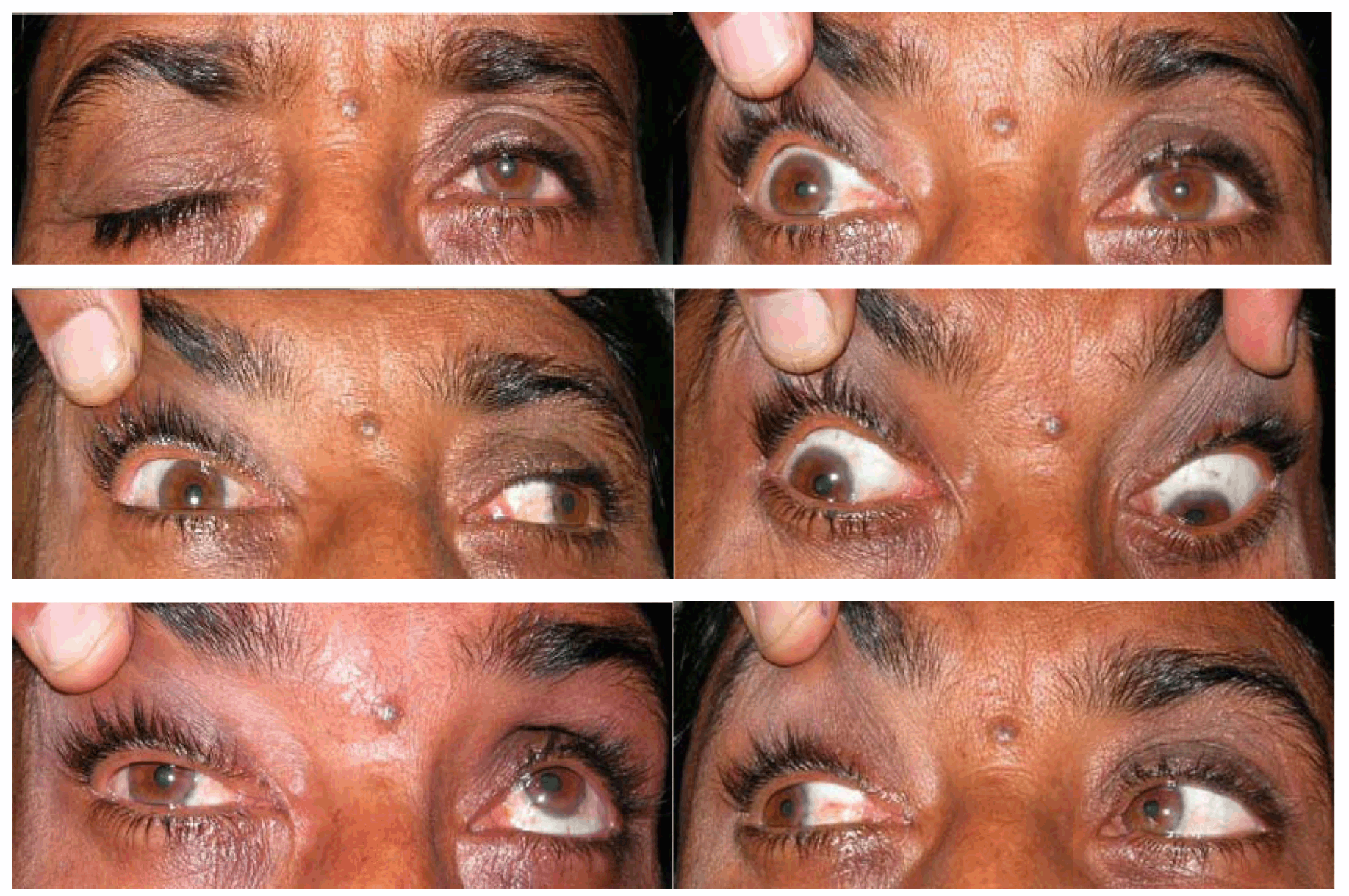
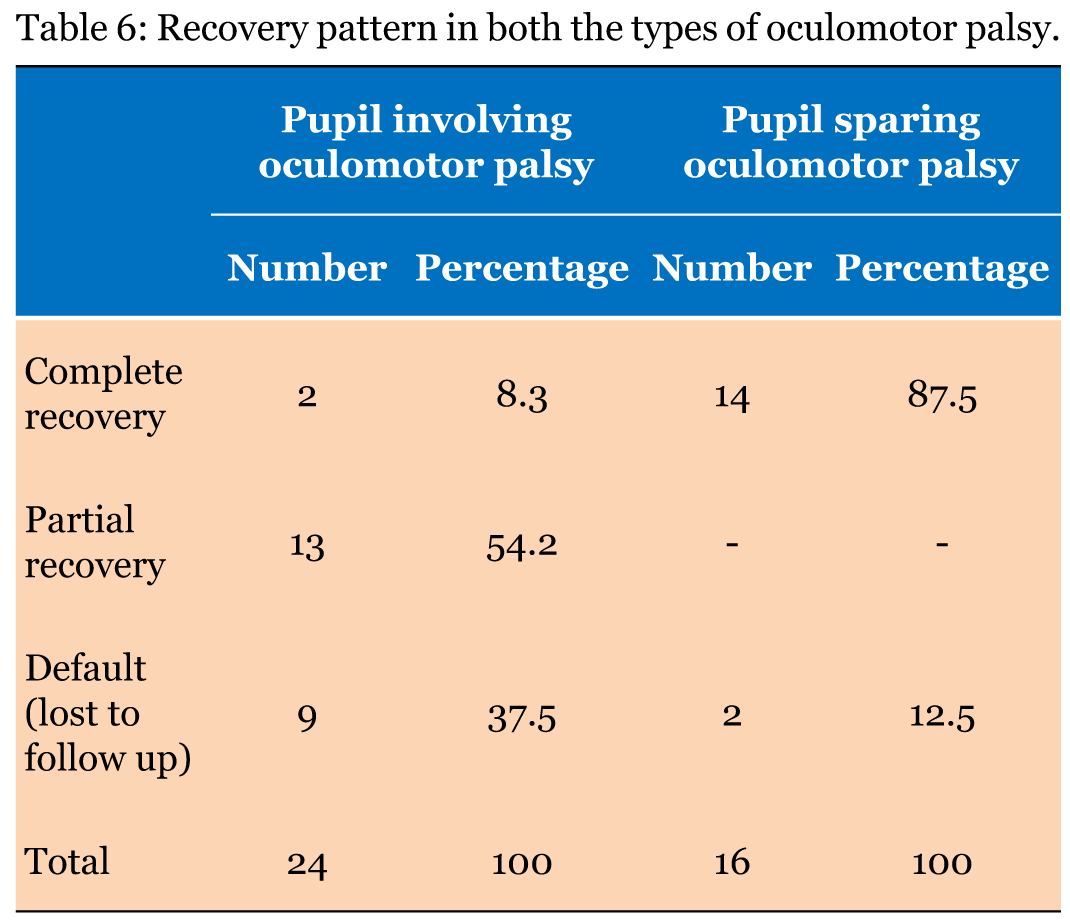
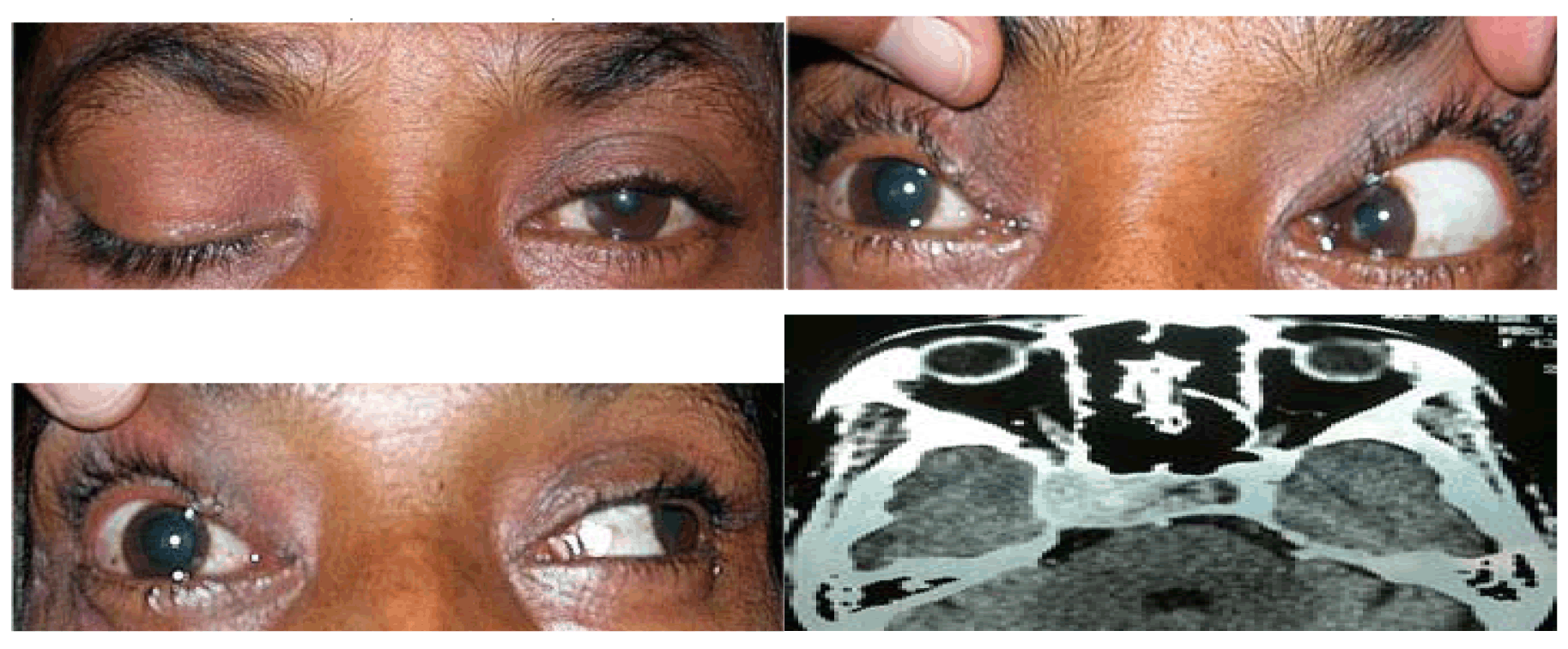
Total 40 subjects were included in the study with oculomotor nerve palsy, the male to female ratio was 1:0.8. Majority of patients belonged to age group <40 years. The mean age of the patients with oculomotor nerve palsy was 46.35 years. In 37 (92.5%) patients, oculomotor nerve palsy was unilateral whereas in 3 (7.5%) patients it was bilateral. All cases with bilateral oculomotor nerve palsy had lesion located in the midbrain involving the oculomotor nucleus. Table 1 gives demographic and clinical characteristics of all the 40 patients enrolled in the study. Eighty percent cases had a specific etiology whereas in others a diagnosis of cranial neuritis or neuropathy of undetermined etiology was made. In this series, 23 (57.5%) cases had isolated third cranial nerve palsy, the causes being microvascular ischemia (20%), post-traumatic (17.5%), undetermined etiology (20%), neurotuberculosis (12.5%) and intracranial aneurysms (7.5%). (Table 2) Ten cases had multiple cranial nerve palsy, half (50%) of them were diagnosed to have idiopathic orbital inflammatory disease (IOID) while remaining (10%) had intracranial space occupying lesions (ICSOL), tubercular basal meningitis (20%), orbital mucormycosis (10%) (Figure 1) and subarachnoid hemorrhage (10%). (Table 3) There were three cases of bilateral oculomotor nerve palsy all of which had nuclear lesion. These consisted of one case each of Nothnagel syndrome (1), nuclear lesion with AINO (Figure 2) and dorsal midbrain syndrome. (Table 4) Five (12.5%) patients had mild ptosis whereas 11 (27.5%) and 24 (60%) cases had moderate and severe ptosis, respectively. Complete ptosis was mostly seen in isolated cases of the third cranial nerve palsy. (Table 5) Pupillary involvement was noted in 60% cases, while 40% cases had pupil sparing isolated oculomotor nerve paralysis. (Figure 3) Majority of patients (54.2%) with pupil involving oculomotor nerve palsy had only partial recovery, while majority of patients (87.5%) with pupil sparing paralysis had complete recovery. (Table 6) Pupillary involvement was noted in all cases belonging to intracranial aneurysms, intracranial neoplasms, (Figure 4) neurotuberculosis, post-traumatic and idiopathic orbital inflammatory groups. All the cases belonging to microvascular ischemia and undetermined etiology groups had pupil sparing oculomotor nerve palsy. Most patient's with microvascular ischemia and undetermined etiology groups had complete recovery while patients in post-traumatic, neurotuberculosis and miscellaneous groups had only partial recovery. Patients with orbital inflammatory group had variable recovery. (Table 7) In the present study, 8 (20%) patients referred for further management were lost for subsequent follow-up. | ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
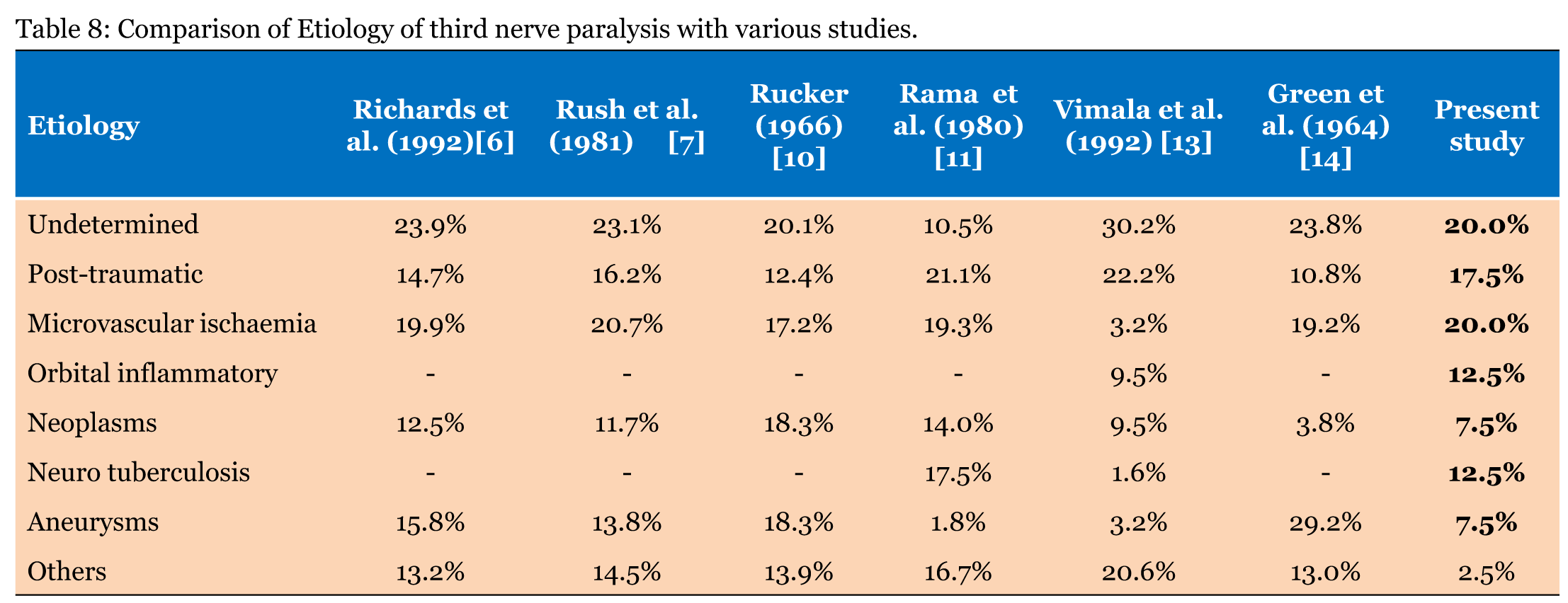
Oculomotor nerve palsy can result from lesions located anywhere from the oculomotor nucleus to the termination of the third nerve in the extraocular muscles within the orbit. Age of the patient, characteristics of oculomotor nerve palsy (partial or complete), presence of associated symptoms and signs of neurological involvement aid in diagnosis and management of oculomotornerve dysfunction. Recent advances in noninvasive neuroimaging facilitate early diagnosis; however, management of a patient presenting with an isolated third nerve palsy remains a challenge. [4] In the present case series, microvascular ischemia (20%) and head injury (12.5%) were significant causes for isolated oculomotor nerve as found in most of the earlier studies. Microvascular ischemia group had the best recovery which was comparable to previous studies. Trobe et al. suggested an approach to manage pupil sparing oculomotor nerve palsy based the relative deficit in pupillomotor and extraocular muscle function. He divided patients into three groups: (1) patients with a normal pupillary sphincter and completely palsied extra-ocular muscles. Such patients should not have cerebral angiography if they are aged 50 or more; (2) patients with a normal pupillary sphincter and incompletely palsied extraocular muscles. Such patients should have angiography, particularly if the inferior oculomotor division is spared; (3) patients with a subnormal pupillary sphincter and completely palsied extraocular muscles ("relative pupil-sparing"). Such patients should have angiography unless they have clear-cut vasculopathic findings. [5] Post-traumatic oculomotor nerve palsy accounted for 17.5% of total cases as compared to Richards et al. (14.7%) and Rush et al. (16.2%). [6] [7] The pathogenesis of oculomotor palsy in head injury is sufficiently well documented. [8] The etiology of third cranial nerve palsy remained unknown in about 20% cases comparable to earlier studies. Rucker et al. found 21% while Krishna et al. found 18% cases due to undetermined etiology. No definite explanation could be offered for this. [9] [10] In our study 70% cases were ≤50 years of age which is comparable to Menon et al. who found 71% incidence in 11–40 years age group. The distinctive feature of the present study was the recognition of orbital inflammatory diseases as a specific and significant cause of oculomotor nerve palsy (12.5%). In most of the earlier studies, these etiologies were considered as miscellaneous causes except for series Vimala et al. series, who used ultrasonography as an investigative tool in the diagnosis of these cases and found similar results to present study (9.5%). Neurotuberculosis presenting as basal meningitis accounted for 12.5% cases in the present study. An earlier study from South Indian by Rama et al. (17.5%) had comparable results owing to high prevalence of tuberculosis in the area. [11] Neurotuberculosis emerged as a significant cause in the present study which reflects the continued prevalence of tuberculosis in this part of the region inspite of effective national programme for control of tuberculosis. Majority of patients with pupil sparing oculomotor nerve palsy had complete recovery as compared to patients with pupil involving oculomotor nerve palsy. Idiopathic orbital inflammatory disease should be categorised as a specific disease entity, which has prompt response to treatment with systemic steroids although residual visual loss persists if the optic nerve is involved. Ptosis, in connection with oculomotor nerve palsy may be of different degrees, as shown in the present study. A careful objective assessment of mild ptosis is necessary in patients with mild ptosis as most of these patients are unaware of this. The overall recovery of oculomotor nerve palsy in the present study (72.5%) was better compared to earlier studies by Singh et al. (50%). [12] A comparative analysis of etiology of oculomotor nerve palsy with other similar studies is given in Table 8.[13] [14] A small number of patients investigated in the present study is the main limiting factor of this series; however, such a limitation may be counterbalanced by the advantage provided by the methodological approach. The course of ophthalmoplegia and anisocoria could have been more precisely studied had the patients been followed up at closer intervals. | ||||||
| ||||||
|
Conclusion
| ||||||
|
Isolated oculomotor nerve palsy which is a predominant mode of presentation has a good recovery rate. In conclusion, we recommend that patients with oculomotor nerve palsy be carefully clinically examined in close collaboration with other specialists, especially where sophisticated complementary investigations are impossible. | ||||||
|
Acknowledgements
| ||||||
|
The authors are very grateful to Dr. S.M. Shivashankariah (Department of Ophthalmology) for his constructive comments and advises throughout the execution of the study. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Maraiah Pradeep Kumar – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Revising it critically for important intellectual content, Final approval of the version to be published Undrakonda Vivekanand – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Shashikiran Umakanth – Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Yashodhara BM – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 Maraiah Pradeep Kumar et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Authors
| |||
| |||
| |||
| |||
| |||